Prof. asoc. Dr. Stefan Gress
Plastic & Aesthetic Surgeon





Labiaplasty / Labia Reduction
Professor Gress is one of the
top specialists in female intimate surgery internationally
What would you like to find out more about?
Labiaplasty
All important information
In most cases, the decision to undergo a labia reduction can be attributed to a combination of physical and psychological issues:
Functional reasons
(pain, chronic skin irritation, invagination during sexual intercourse, etc.)
Aesthetic reasons
(hesitation to get naked, negative impact on sex life, etc.)
For many women, the anatomic variations of their genitals can be a source of significant suffering. Hormonal influences, weak tissue, genetic factors, or age-related changes may cause these deviations in shape. Large labia minora and sagging labia majora are found to be particularly distressing.
Functional problems, such as pain when wearing tight-fitting clothing, playing sports (horse riding, jogging, cycling), invagination of the labia minora during sexual intercourse, and hygiene issues, can motivate women to opt for surgical correction. Another reason to undergo a genital correction procedure is psychological distress, which can be significant in some patients, caused by restrictions on the patient’s sex life.
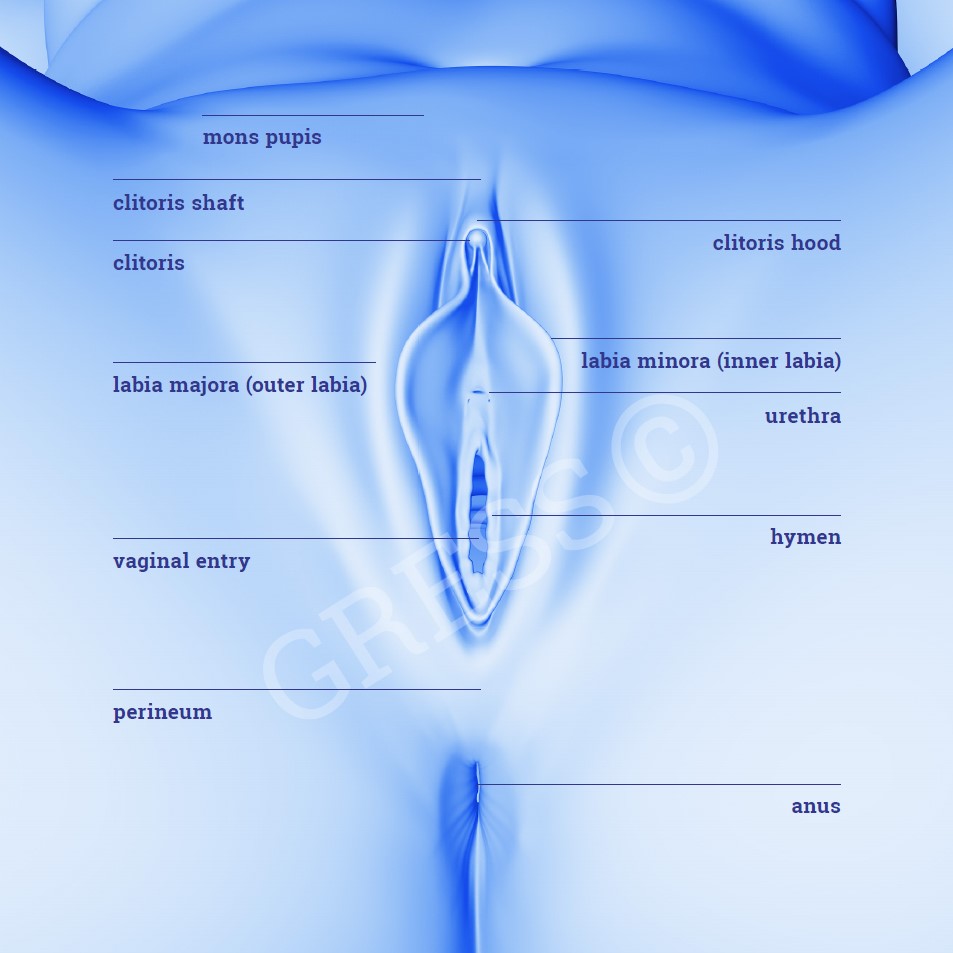
Here is some important medical information about the function and structure of the labia:
The small (inner) vaginal lips seal the vaginal opening and prevent infections developing inside the vagina, and other conditions.
The large (outer) vaginal lips enclose the small vaginal lips and offer mechanical protection.
The clitoris is the only organ that purely serves the purpose of sexual stimulation
The labia cover and seal the vaginal opening, protecting the vagina from drying out and stopping foreign bodies and pathogens from making their way in. Additional mechanical protection is offered by the fat pads of the labia majora.
The labia minora extend from the mons pubis towards the anus, encompassing the clitoris and the vaginal opening. The part of the labia adjacent to the clitoris is also referred to as the “clitoral hood”. In terms of morphology, the labia minora are equivalent to the foreskin of the penis. They are of secondary importance for sexual stimulation.
The term clitoris is commonly used to refer to a small, pea-shaped anatomical structure located a little above the urethral opening. However, the clitoris is not spherical but rather band-like in shape, similar to a small penis, with only the tip (glans clitoris) protruding and being visible. Its shaft (corpus clitoris) extends in a deeper layer across the pubis and is thus not visible. The clitoris is responsible for sexual stimulation.
We will do our best to ensure that you are given a delicate work of art that fully lives up to your wishes and expectations.
We usually aim for the labia minora to be covered by the labia majora, but other shapes and variations can also be achieved.
The “ideal” appearance
in our culture, anything that sags or hangs shapelessly is often perceived as unattractive. Since shaving public hair has become routine for most women today, the shape and appearance of the genitals are unveiled, also regrettably revealing any less appealing details.
Even though the idea of what the perfect labia should look like varies greatly from woman to woman, of course, there is one “look” of the outer female genital area that most patients consider to be ideal:
When it comes to what constitutes the “perfect shape”, the labia minora have a slightly curved contour with a firm clitoral hood. When the legs are closed, the labia minora are almost completely covered by the labia majora.
For many women, however, the labia minora hang down limply and protrude beyond the cover of the labia majora.
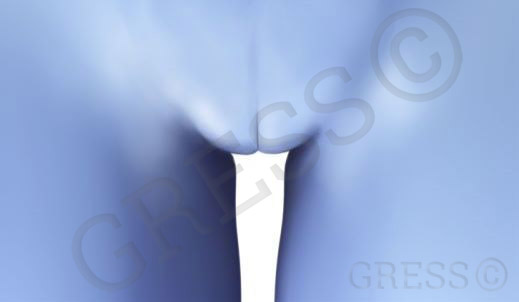
well-shaped labia majora, resembling the shape of a closed shell.
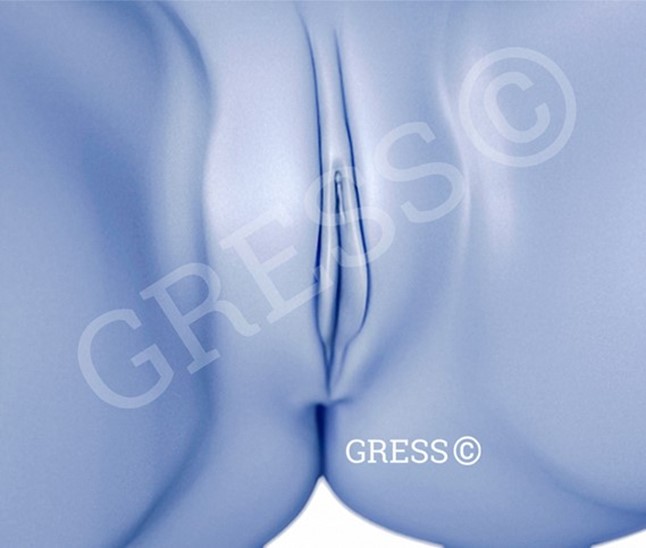
The main concern here is to analyze the starting situation, particularly with regard to the desired result. In which areas are the labia minora enlarged? Purely below the clitoris or also above it, in the shaft part of the clitoris? Is there clitoral protrusion or is the clitoris in a normal position, etc.?
If the labia minora are very long – a condition called labial hypertrophy – they are no longer covered by the labia majora. Labia minora are typically enlarged along their entire length, i.e. the part above the clitoris, the area adjacent to the clitoris (clitoral hood) and the part below the clitoris. An isolated hypertrophy of the lower part alone is rare.
In cases where all sections are enlarged (the most common form), all parts have to be corrected in order to achieve a balanced and aesthetically appealing result.
Attention should also be paid to the position of the clitoris itself:
In some cases, the clitoral glans can protrude to a great extent. This is referred to as clitoral protrusion. In cases where full coverage of the labia minora by the labia majora cannot be achieved with the labia reduction procedure alone, surgical correction of clitoral protrusion is advisable.
The procedure is typically performed under local anesthesia; however, analgosedation (twilight sedation) or general anesthesia are also available on request. Prior to surgery, we will sit down with you to decide on every detail of the changes you desire. This involves us taking exact measurements to determine how much skin and tissue needs to be removed to achieve a perfect result that is as symmetrical as possible.
To make the necessary incisions, we use a radiofrequency surgical device (similar to a laser scalpel) to enable very precise and tissue-conserving surgery with minimal bleeding. This results in a markedly improved and significantly accelerated healing process. The edges of the incision wound are closed carefully with fine, absorbable sutures.
The procedure
The best surgical technique for you is selected based on your desired result. This does, however, depend not only on your expectations of the result, but also on your starting situation.
There are four different options: labia reduction along their entire length, or purely below the clitoris, with or without tightening the clitoral hood, with or without correcting the position of the clitoris, etc.
We differentiate between four techniques used for the reduction of the labia minora, depending on the examination findings and the starting situation:
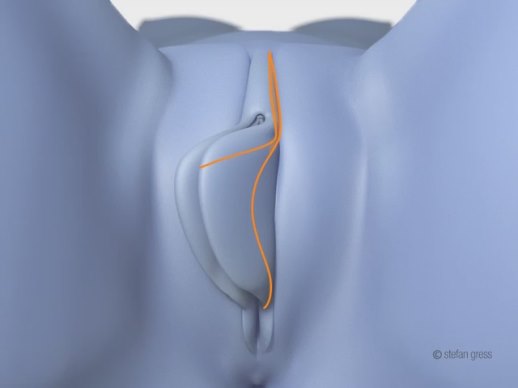
A. Composite Reduction Labiaplasty
- Reduction of the labia minora in all three sections
- Correction of the clitoral position in case of a bulging clitoris (clitoral protrusion)
- Additional upward tightening of the clitoral hood
The excess tissue in the areas highlighted in orange is removed. Clitoral protrusion is corrected by lowering the protruding clitoral glans. To tighten the clitoral hood, both skin flaps are tightened downwards and the clitoral hood is tightened upwards.
B. Reduction Of The Labia Minora In All Sections (with Correction Of The Clitoral Position)
- Reduction of the labia minora in all three sections
- Correction of the clitoral position in case of a bulging clitoris (clitoral protrusion)
This technique is almost identical to the variant described above. In this case, however, no skin area is removed above the clitoris
C. Reduction Of The Labia Minora In All Sections (without Correction Of The Clitoral Position)
- Reduction of the labia minora in all three sections
Removal of the excess tissue (highlighted in orange). Unlike the procedures described above, only a downward tightening of the clitoral hood is performed; there is no correction of the clitoral position and no additional upward tightening of the clitoral hood. Two triangles of skin are removed from the sides to prevent engorgement of the tissue that would otherwise develop as the flaps are pulled downwards.
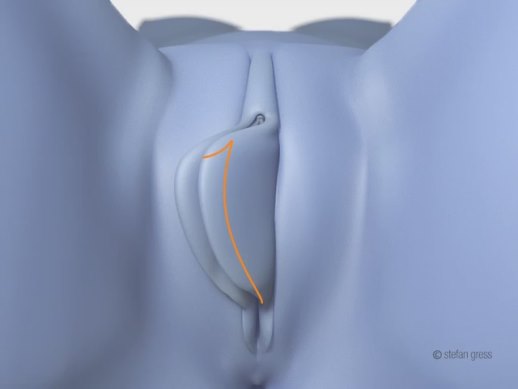
D. Reduction Of The Labia Minora Only In The Area Below The Clitoris
This procedure should only be considered in cases involving isolated enlargement of the labia minora limited to the part below the clitoris. However, these cases are rare.
Excess tissue highlighted in red is removed.
As labia reduction surgery is performed under local anesthesia, extensive preparation is not required. It is important that you do not take any blood-thinning medications (e.g. aspirin, etc.) 14 days prior to the surgery.
Before the surgery:
If the procedure is being performed under local anesthesia, no special preparation is required. If the procedure is being performed under general anesthesia or twilight sedation, you should fast, i.e. refraining from eating, drinking, and smoking, for at least six hours prior to your surgery.
You should stop taking medications that affect coagulation, e.g. aspirin 100 mg, etc., 14 days prior to the surgery. Please completely shave your genital area before the procedure.
You will be given a delicate work of art. You need to protect it. Avoid mechanical friction as much as possible for six weeks after the procedure. Please also note the following:
After the surgery:
After the surgery, you can rest at our practice.
Please do not drive home or back to your hotel yourself. Get someone to pick you up or we can call a taxi for you. Cool the area and rest. You should walk as little as possible. You may experience a mild burning or pressing sensation, especially during the first night. This is normal. However, some patients feel it more than others and, despite the pain medication prescribed by us, a few patients may experience significant discomfort. The sensation typically disappears or greatly improves after the first night. On the first postoperative day, the wound is checked and the dressing is changed at our practice.
After the third day, you can start showering again, but may only use clear water and no soap during the first week. The sutures are absorbable and do not need to be removed. Absorption of the suture may sometimes be associated with severe itching, which can be alleviated by using special creams or ointments.
The surgery will only affect your daily activities for a short time. Depending on your profession, you may be able to return to work as early as two to three days after surgery. It is very important that you try to avoid any friction and forces acting on this area for six weeks following the procedure: no sexual intercourse, jogging, cycling, horse riding, etc.! Likewise, tampons may only be used again after this period of time.
Immediately after surgery, you should wear close-fitting underwear that you can pull firmly upwards to apply some pressure on the area. This helps prevent excessive swelling and reduces the risk of postoperative bleeding. Then from the first day after surgery, you will feel more comfortable wearing loose clothing.
To optimize the healing process, you should place a compress between the labia so that they do not touch. You should do this over a period of two weeks. After this time, you should firmly squeeze the labia along their entire length between your thumb and index finger. You should do this two to three times a day over a period of four weeks. This will encourage any swelling to subside more quickly and improve scar healing. However, be careful not to rub or massage the labia.
You will be provided with the cell phone number of Prof. Gress so that you can contact him any time should you have any questions or experience an emergency.
Prof. Gress has published most of his medical publications with Springer Verlag.
His textbook on correcting the outer female genital region entitled „Aesthetic and Functional Labiaplasty“ was published in 2018.
This book describes his techniques for reducing the labia minora, primarily the “composite reduction labiaplasty”, and techniques for correcting the labia majora and the mons pubis. This textbook is now the standard for colleagues in this field throughout the world.
Publications by Prof. Gress:
(click for further information)
Good to know
Frequently asked questions about labia reduction
How many appointments do I need?
For outpatient operations, you will need a total of three appointments:
consultation/preliminary examination, surgery, and a follow-up examination the morning after the operation. The consultation and surgical procedure may not take place on the same day. There has to be an interval of at least 24 hours between the initial consultation and the surgery itself.
After the operation, you should spend the night in Munich. We will be glad to help you find a suitable hotel.
We will be glad to help you find a suitable hotel of any kind. We have a partnership with Hotel Vier Jahreszeiten Kempinski, Munich, which means our patients are offered more favorable rates. They should, however, refer to our practice when booking the hotel or make the booking with our assistance .
Traveling from afar
We offer to accommodate consultation and surgery in one stay for patients who have a long journey to get to Munich. This would involve arriving the day before surgery for a consultation and physical examination with Prof. Gress. The procedure is performed the next day and the follow-up examination is carried out the day after. You would therefore need to spend two nights in Munich.
Hotels
We will be glad to help you find a suitable hotel of any kind. We have a partnership with Hotel Vier Jahreszeiten Kempinski, Munich, which means our patients are offered more favorable rates. They should, however, refer to our practice when booking the hotel or make the booking with our assistance .
Sport
When can I resume sporting activities?
It is extremely important that you avoid any strong friction in the genital area for at least six weeks to support the healing process. Sexual intercourse, horse riding, jogging, cycling, etc. are prohibited during this time! We recommend that you use a cross trainer or stepper if you would like to exercise during this period, as the leg position is somewhat wider, meaning there is no friction.
Sexual intercourse
When can I resume sex?
Sexual intercourse is to be strictly avoided during the first six weeks after surgery as the significant friction would open up the wound edges again. As long as the sutures do not get in the way, you can have oral sex again four weeks after surgery.
Showering, water, soap
What intimate hygiene is best for me after surgery?
You can take a shower after two days, but may only use clear water for one week. Please only use pH-neutral products. Do not take a bath as this would soften the wound edges! We only use absorbable sutures. Unpleasant itching may be experienced along with suture absorption. We recommend that you use Bepanthen ointment or pure Aloe Vera gel to alleviate this symptom.
Swimming
When can I resume swimming?
You should avoid chlorine-treated water in public swimming pools for six weeks. You are allowed to swim again in lakes or the sea after four weeks.
Scar creams
Are scar creams recommended?
Since scars in the genital area generally tend to heal very well, these are usually not necessary.
Sauna, sun bed
When can I be in the sun or use a sun bed again?
Sun and UV rays have a negative impact on scar healing. Please ensure that the area is protected from them for a period of six months.
Pain
Generally speaking, the injection is not painful.
Periods
Having your period on the day of surgery does not constitute a problem.
Childbirth
Does labia reduction have an impact on giving birth?
No. If you become pregnant after the procedure, you can give birth naturally. The surgery does not affect the process of giving birth, and conversely, giving birth has no negative impact of the result achieved with the procedure.
Clothing
What kind of clothing is advisable?
On the day of surgery, please bring along firm-fitting underwear to wear after the procedure to apply some pressure to the area. This helps prevent excessive swelling and reduces the risk of postoperative bleeding. Then from the first day after surgery, you will feel more comfortable wearing loose clothing.
Shaving
Please completely shave your genital area before the procedure.
Working
You can return to work the day after the procedure.
Your contribution to the healing process
What can I do to promote healing?
Take the medications as prescribed by us. You will be given a painkiller that reduces swelling plus an antibiotic. Please avoid any kind of friction for at least six weeks after surgery! To aid the healing process, place a compress between the labia during the first two weeks after surgery so that they do not touch. After this time, you should firmly squeeze the labia along their entire length between your index finger and thumb, even if it is painful to do so. This promotes scar healing and accelerates the time it takes for the swelling to subside. You should do this two to three times a day over a period of three to four weeks. We will show you exactly how to do this on the day of your first wound check.
Laser or scalpel?
We perform the procedure using a radiofrequency surgical device. Similar to a laser, the tissue is cut using thermal energy; however, the tissue is separated through contact between the wire and the skin, instead of a light beam. The advantage is that any trembling of the hand is not transferred to the incision line, as is the case with a laser. It is virtually impossible to perform this procedure using a scalpel as a precise incision line cannot be achieved, given the looseness of the tissue.
Final result
When will I be able to see the final result of the labiaplasty?
Around 80% of the swelling will have subsided within six weeks or so. The rest of the swelling is barely visible but will disappear relatively slowly and it may be up to six months before it has subsided completely. After this, there will be no further changes and the end result will be achieved.
Sutures, stitches
The stitches are made of absorbable sutures and do not need to be removed. They can, however, start to itch after a few days. If this happens, you can apply a sterile ointment (e.g. Bepanthen) to the wound to relieve the itching or have the sutures removed from 12 days after the labiaplasty (by us or by your gynecologist or family doctor).
Simultaneous correction of labia minora and majora
It is not possible to perform a reduction of both the labia minora and majora in one single surgery. The healing process is extremely complicated which would have a negative impact on the result. There should be an interval of around six months between each procedure.
A reduction of the labia minora can, however, be combined with a procedure to fill the labia majora with autologous fatty tissue (lipostructure).
Risks
Risks and potential complications
After the procedure, there will be some swelling which will generally start to subside gradually after the first or second day. Around 80% of the swelling will subside within the first six weeks after surgery; the remaining swelling takes comparatively longer to disappear, in some cases up to six months. You may experience minor bruising. You can help prevent this by wearing firm-fitting underwear immediately after the procedure to apply some pressure to the area.
Varying levels of pain can also be expected, especially during the first night after surgery. You should, however, be able to tolerate this quite well if you take the pain medication prescribed by us.
Wound healing may be disturbed, especially if the area is exposed to excessive forces too early. It is therefore crucial that you avoid any kind of strong friction (e.g. sexual intercourse) during the first six weeks after surgery. Likewise, you should not use tampons during this period.
Once the wound has healed, scars in the genital area are usually very inconspicuous and hardly noticeable, even on close inspection. Theoretically, scars can develop to become thick, reddened, or painful. However, this has so far not been observed in the genital area. Special ointments would help in this case. To promote good scar healing, you should squeeze the scars between your fingers two weeks after surgery. We will show you exactly how to do this at our practice.
Sensory disturbances are not to be expected. You may experience some numbness or sensitivity to touch in the beginning, but this will disappear once the wound has fully healed. When a correction of a bulging clitoris (clitoral protrusion) is performed, the clitoris is shifted closer to the vaginal opening, which may enhance sexual stimulation.
Postoperative bleeding, asymmetries, wound infections, etc. are very rare.
Costs and operating time
The costs for labia surgery depend on the type and duration of the procedure and range between EUR 2,800 and EUR 5,500; fees for complex reconstructions are somewhat higher.
If the procedure is being performed under twilight sedation or general anesthesia, the anesthetist fees are charged in addition to the usual cost of the surgery.
- Labia minora reduction purely below the clitoris, approx. 1-1.5 hours operating time EUR 3,000
- Labia reduction on one side only, approx. 1-1.5 hours operating time EUR 2,800
- Labia reduction along their entire length without clitoris correction, approx. 2 hours operating time EUR 4,500
- Labia reduction along their entire length with correction of clitoris protrusion, approx. 2.5 hours operating time EUR 5,500
- Composite Reduction Labiaplasty, approx. 2.5 hours operating time EUR 5,500
If the procedure is being performed for cosmetic reasons alone, VAT of 19% is applied to the costs, in accordance with German law. If the main reason for the operation is due to medical impairments, e.g. pain during sexual intercourse or playing sport, a deflected urinary stream, skin irritation, or frequent bladder or fungal infections, VAT is not applicable. Before the day of the surgery, you need to provide confirmation from your gynecologist that there is a medical indication for surgery. A brief written confirmation that the reduction of the labia minora is being performed for medical reasons is sufficient.
The fee for the operation must be settled before the day of the surgery. A deposit of EUR 500 is required to secure an appointment for surgery Operating time and costs.
Insurance
Absorption of costs by health insurance companies
Statutory health insurance providers shall only bear the costs, if at all, in accordance with their rates and after examination by the medical service. We do not work in partnership with any of the statutory insurance companies.
Private insurance companies, on the other hand, are less restrictive and cover part or all of the costs if there is a medical indication. A medical indication exists if the patient is experiencing functional impairments, such as pain during sexual intercourse, playing sports, wearing tight clothing, hygiene problems with skin irritations, etc. Physical impairments can also represent an indication for surgery.
It is advisable to inquire in advance with your insurance company whether or to what extent the procedure is covered.
Financing
Please understand that we are unable to provide any financing ourselves. However, MEDIPAY has been our reliable partner on this matter for many years now. You can find all the relevant information by clicking on the following link www.medipay.de.
Individual information
You can request further information or arrange an appointment here. This is non-binding information free of charge. We have set up a telephone advice service for you. Call +49 (0) 89 24 22 39 22 for advice on your own surgical needs. This personal advice service is non-binding and free of charge.

Best Results
by specially developed, internationally leading surgical technique “Composite Reduction Labiaplasty”

Greatest Experience
With the most operations in
the female genital
area worldwide

Media Partner
First point of contact for international media for all questions relating to intimate surgery
Prof. Dr. Gress
Experience makes the difference
- More than 6700 procedures in the female genital area
- Over 20 years of experience
- Inventor and developer of the “Composite Reduction Labiaplasty”
- Internationally recognized top specialist
- Author of the international textbook “Aesthetic and Functional Labiaplasty” (Springer Publishers)
- Professor and Lecturer in Plastic Surgery

„Pioneer of female genital surgery“

„The Vagina Picasso“

„The labia pope of Germany“

Memberships
In the most important national and international specialist societies

American Society of Plastic Surgeons

Deutsche Gesellschaft der Plastischen, Rekonstruktiven und Ästhetischen Chirurgen

International Confederation for Plastic, Reconstructive and Aesthetic Surgery

International Society of Aesthetic Plastic Surgery

The Aston Baker
Cutting Edge
Aesthetic Surgery
Symposium
2018, New York
Faculty Member
The greatest honor for
a Plastic Surgeon
Aesthetic and Functional Labiaplasty
The international Textbook
written by Prof. Gress

Published in January 2018 by Springer Verlag, it has developed into an international bestseller and standard work in plastic surgery.